Menopause, Hunger, and the Brain
Why things changed—and why it was never about willpower
When I did weight loss surgery, about 80 percent of my patients were women.
There were many stories I heard, but there was one that repeated itself with such consistency that you couldn’t ignore it. When menopause—or even perimenopause—arrived, weight would follow. Not gently. Not politely. It would accumulate in a way that felt unfamiliar, almost unfair.
Some of these women had struggled with weight before. Others had never given it much thought. They had lived their lives, eaten reasonably well, stayed active, raised families, built careers. Then something shifted.
Not overnight—but steadily enough to feel unmistakable.
And the explanation they were given was always the same.
“Your metabolism is slowing down.”
It sounded scientific. It sounded final.
It just wasn’t the whole story.
What We Missed
What we know now is more interesting—and far more useful.
Estrogen does not just affect hair, hot flashes, or the vaginal epithelium. It has a quiet but powerful role in the brain. Specifically, it acts on the hypothalamus, that small but commanding region that helps regulate hunger, satiety, and energy balance.
When estrogen is present, it helps keep the system in tune.
When it declines, the signal changes.
And when the signal changes, something women often describe as food noise begins to rise.
Not because they’ve changed.
Because the system has.
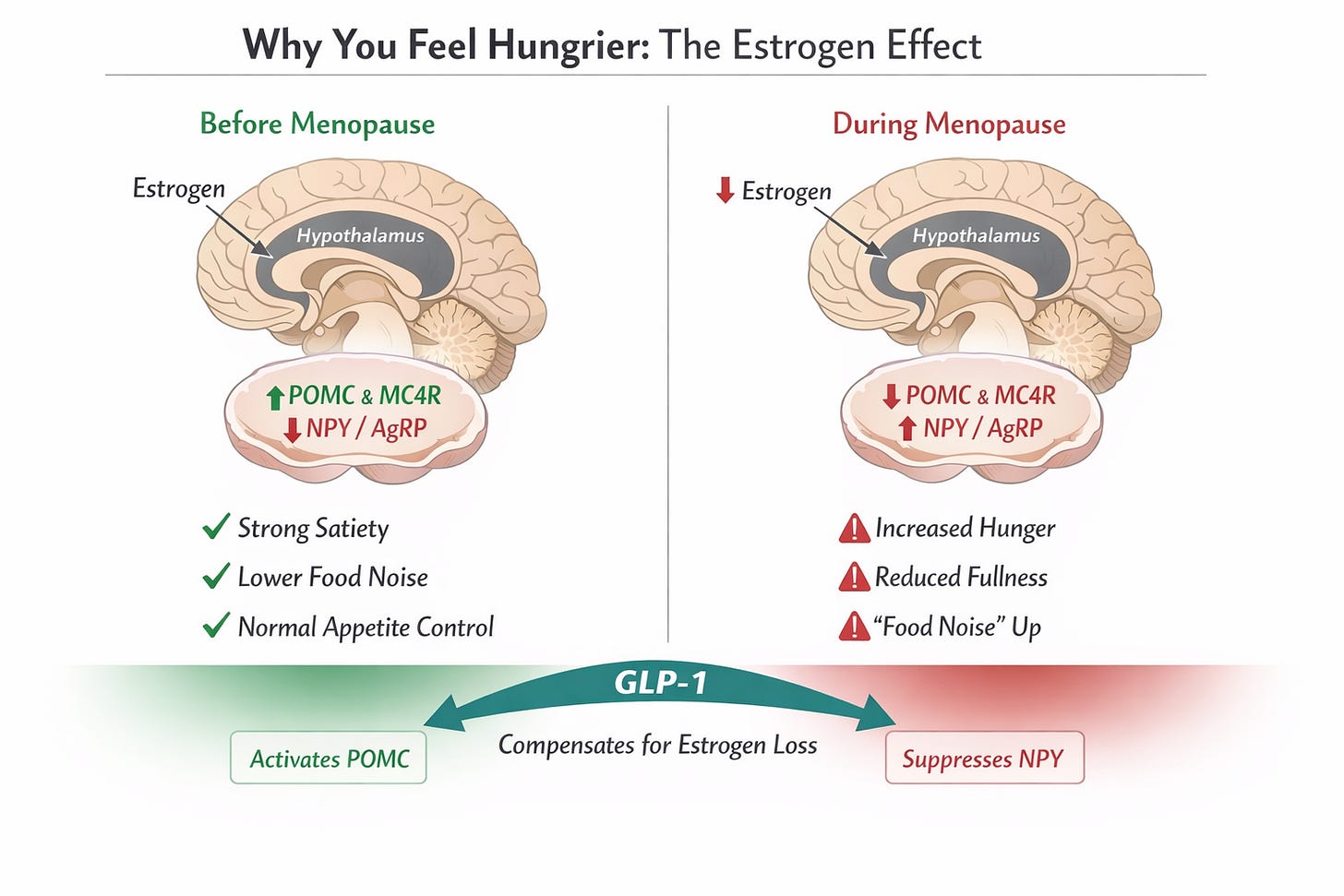
The Brain Before and After Menopause
Here is the simplest way to understand it.
You don’t need to memorize the names—but they tell a story.
On one side, you have POMC—the signal that says, you’ve had enough. It promotes satiety, helps you feel full, and allows you to walk away from the table without negotiation.
On the other side, you have NPY—the signal that says, eat now. It increases hunger, sharpens attention toward food, and makes eating feel more urgent.
Estrogen, quietly and effectively, helps keep these in balance.
It supports the fullness signal.
It restrains the hunger signal.
When estrogen declines, that balance shifts.
The “eat” signal grows louder.
The “stop” signal becomes less convincing.
And the experience of eating changes.
Why It Feels Different Before It Looks Different
One of the most striking things women tell me is this:
“I don’t think I’m eating that much more—but I’m thinking about food all the time.”
That matters.
Because appetite isn’t just behavior—it’s perception. It’s the internal conversation that happens before you ever pick up a fork.
Studies have shown that hunger increases and fullness decreases during menopause—even when intake hasn’t yet changed. The system becomes less efficient.
And that’s when frustration begins.
Because from the outside, it looks the same.
But from the inside, it feels completely different.
The Part We Should Have Said Sooner
There is a part of this conversation that deserves some honesty.
For years, women were told to endure menopause. To manage symptoms. To tolerate the changes.
And when weight increased, when hunger changed, when the body felt unfamiliar—they were told to try harder.
Eat less. Move more. But we were missing something fundamental.
Estrogen is part of the system that regulates appetite. So when that system changes, the experience changes. And instead of acknowledging that—we blamed the patient.
That wasn’t just incomplete. It was unfair.
What Estrogen Replacement Really Does
When we talk about estrogen replacement, the conversation is often limited to hot flashes and sleep. But there is another layer.
Estrogen helps restore some signaling in the brain that menopause disrupts. It supports the pathways that promote satiety and helps quiet the ones that drive hunger.
It doesn’t turn the clock back. But it can help the system function more like it used to. And importantly—it does not cause weight gain.
That idea has lingered far longer than it should have.
How This Fits Into Modern Treatment
Now, medicine evolves. What we once treated as symptoms, we now understand as systems. Hormone therapy is no longer just about symptom relief. It is part of a broader understanding of how hormones influence the brain, metabolism, and long-term health.
We are beginning to see menopause not as something to endure—but as something to manage thoughtfully. Not aggressively. Not reactively. But intelligently.
And Then There Is GLP-1
There is another piece to this story, and it is impossible to ignore.
GLP-1 medications act on the same appetite centers in the brain. They enhance the fullness signal and quiet the hunger signal.
But here’s the part that matters:
Estrogen appears to improve how well GLP-1 works.
That includes both:
the GLP-1 your body naturally produces
and the medications we now use clinically
So menopause may not only reduce estrogen—it may also reduce the brain’s responsiveness to satiety itself. Which helps explain why things feel harder.
And why, for some women, restoring part of that system—through hormones, through GLP-1, or both—can feel like turning the volume down on something that had been getting louder for years.
Where This Leaves Us
This isn’t about telling every woman what she should do.
It’s about giving her the right explanation.
Menopause is not a failure of willpower.
It is not simply a slowing metabolism.
It is a shift in how the brain regulates hunger.
And once you understand that—you stop blaming yourself. You start asking better questions. And you realize something important: The system changed. Not you.
1.mTOR Signaling in the Arcuate Nucleus of the Hypothalamus Mediates the Anorectic Action of Estradiol.The Journal of Endocrinology. 2018. González-García I, Martínez de Morentin PB, Estévez-Salguero Á, et al.
2.Hypothalamic Actions of Estrogens in the Regulation of Energy and Glucose Homeostasis.Reviews in Endocrine & Metabolic Disorders. 2025. González-García I, Xu Y.
3.Estrogen as a Key Regulator of Energy Homeostasis and Metabolic Health.Biomedicine & Pharmacotherapy = Biomedecine & Pharmacotherapie. 2022. Mahboobifard F, Pourgholami MH, Jorjani M, et al.
4.Metabolism Regulation by Estrogens and Their Receptors in the Central Nervous System Before and After Menopause.Hormone and Metabolic Research = Hormon- Und Stoffwechselforschung = Hormones Et Metabolisme. 2016. Coyoy A, Guerra-Araiza C, Camacho-Arroyo I.
5.Estrogen Synthesized in the Central Nervous System Enhances Mc4r Expression and Reduces Food Intake.The FEBS Journal. 2025. Hayashi T, Kumamoto K, Kobayashi T, et al.
6.Estrogen in the Brain - Neuroestrogens Can Regulate Appetite and Influence Body Weight.The FEBS Journal. 2025. Nguyen TT, Kanemoto Y, Kurokawa T, Kato S.New
7.Menopause: A Cardiometabolic Transition.The Lancet. Diabetes & Endocrinology. 2022. Nappi RE, Chedraui P, Lambrinoudaki I, Simoncini T.
8.Weight Gain in Women at Midlife: A Concise Review of the Pathophysiology and Strategies for Management.Mayo Clinic Proceedings. 2017. Kapoor E, Collazo-Clavell ML, Faubion SS.
9.Mechanisms of GLP-1 Receptor Agonist-Induced Weight Loss: A Review of Central and Peripheral Pathways in Appetite and Energy Regulation.The American Journal of Medicine. 2025. Moiz A, Filion KB, Tsoukas MA, et al.New
10.Glucagon-Like Peptide 1 (GLP-1) Action on Hypothalamic Feeding Circuits.Endocrinology. 2025. Hwang E, Portillo B, Williams KW.New
11.Direct and Indirect Effects of Liraglutide on Hypothalamic POMC and NPY/AgRP Neurons - Implications for Energy Balance and Glucose Control.Molecular Metabolism. 2019. He Z, Gao Y, Lieu L, et al.
12.GLP-1 Physiology and Pharmacology Along the Gut-Brain Axis.The Journal of Clinical Investigation. 2026. Beutler LR.New
13.Liraglutide Prevents Body and Fat Mass Gain in Ovariectomized Wistar Rats.Molecular and Cellular Endocrinology. 2024. Rossetti CL, Andrade IS, Fonte Boa LF, et al.
14.Estradiol Modulates the Anorexic Response to Central Glucagon-Like Peptide 1.Hormones and Behavior. 2017. Maske CB, Jackson CM, Terrill SJ, Eckel LA, Williams DL.
15.GLP-1 and Its Analogs: Does Sex Matter?.Endocrinology. 2025. Börchers S, Skibicka KP.
16.Interactions Between Glucagon Like Peptide 1 (GLP-1) and Estrogens Regulates Lipid Metabolism.Biochemical Pharmacology. 2024. Model JFA, Normann RS, Vogt ÉL, et al.
17.GLP-1 Receptor Agonists for Weight Loss for Perimenopausal and Postmenopausal Women: Current Evidence.Current Opinion in Obstetrics & Gynecology. 2025. Mikdachi H, Dunsmoor-Su R.New
18.Impact of GLP1 Agonists on Reproduction.The Journal of Clinical Endocrinology and Metabolism. 2025. Couldwell M, Tidwell AJ, Taylor AE.New
19.GLP-1 Increases Preovulatory LH Source and the Number of Mature Follicles, as Well as Synchronizing the Onset of Puberty in Female Rats.Endocrinology. 2015. Outeiriño-Iglesias V, Romaní-Pérez M, González-Matías LC, Vigo E, Mallo F.
What I Tell My Patients, Family and Friends About Menopause and Hunger